Medications
EVENITY: A Physician’s Perspective
Endocrinologist Dr. Janet Rubin explains how Romosozumab, trademarked under Evenity, affects your bones.
Read More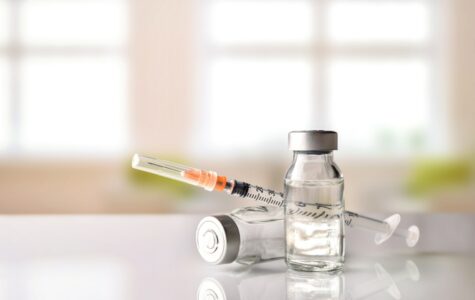
Everything you need to know about osteoporosis medications.
Medications
Endocrinologist Dr. Janet Rubin explains how Romosozumab, trademarked under Evenity, affects your bones.
Read More
Medications
Hear from a leading oral surgeon what to do about the risks of ONJ.
Read More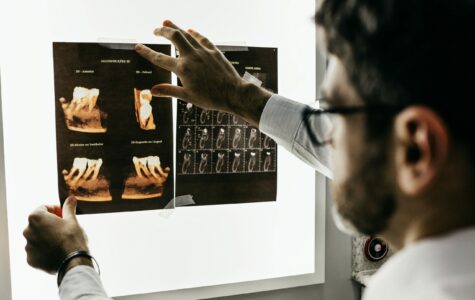
Medications
It is a must-read if you are considering taking it or stopping it.
Read More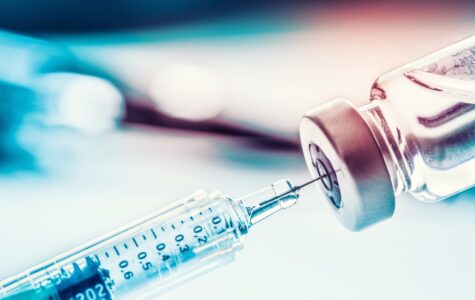
Medications
Bisphosphonates are the most common osteoporosis medication. Learn more about them.
Read More